Your Cart is Empty

After many careful months of carrying your baby, you’re finally ready to meet your little one.
With it comes a laundry list of things you need to prepare in order to support your delivery and your recovery.
It can get overwhelming, but we got you!
In this article, you’ll find everything you need for postpartum care: from what you can expect as you recover to the things you might need before you head to the hospital, so you can take better care of yourself and your baby.
Your type of birth determines your postpartum recovery.
Having a birth plan allows you to predict what you might need after your delivery. Naturally, any surgery requires more time for your body to heal than a vaginal delivery. Still, know that things aren’t completely sure until you’re right in the delivery room. Some mothers might hope for a vaginal delivery but end up getting a C-Section. And these situations happen more often than you think.
Whether or not it’s your first rodeo, allow us to take you through the different types of birth:
Vaginal Delivery
Vaginal delivery is the type of delivery where the baby goes through the birth canal and out to the vagina without assistance of a vacuum extractor or forceps. It comprises all births whether or not they’re assisted with medication.
This goes for moms who choose the epidural and those who don’t. Vaginal deliveries are the easiest to recover from since it doesn’t involve any surgery.
C Section
You’ve probably already heard of a C-Section.
A C-Section is when your baby gets delivered through a cut in your abdomen.
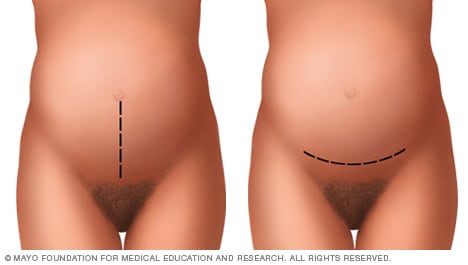
How do you know when a C-section is necessary?

Vaginal Birth after C-Section
Vaginal Birth after C-Section or VBAC usually occurs after your first birth when you’ve had a C-section. Some moms are able to deliver vaginally after C-section. Since C-sections are major surgeries that can be taxing to the body, being able to deliver vaginally is a preferred option.
When attempting a VBAC, you will undergo TOLAC or trial of labor after C- section. You are a candidate for VBAC if you’ve had a low transverse incision on your previous C Section.
The complication that most moms are worried about regarding VBAC is uterine rupture. But don’t fret. The statistics is 1 in 200 moms experience a uterine rupture during VBAC. Despite all the risks that come with a VBAC, the recovery time after a VBAC is still the same as a vaginal delivery, which can last from 4 to 6 weeks.
Vacuum Extraction
A vacuum extraction is done during vaginal delivery to assist the baby out of the birth canal. When the baby is far along the birth canal, a vacuum extractor may be used to help the baby in the following circumstances:
If a vacuum delivery fails, the mother might need to go under C-section. Since the newborn’s head is very delicate, vacuum delivery poses some risks such as head trauma or brain damage.
Forceps Delivery
If vacuum assisted deliveries are used for babies who are far along enough in the birth canal, forceps delivery is when the baby has descended into the birth canal but the mother is unable to push the baby out.
Forceps are metal instruments that look like tongs that are shaped to fit around the baby’s head.
Still, if forceps delivery is unsuccessful, a C-section may be needed.
Whether you got a C-section or vaginal delivery, here are some of the things you can expect after giving birth:
Vaginal and perineum soreness
When you give birth to a human being vaginally, your vagina makes way for it. You must be wondering, can the vagina really stretch that far to make room for the baby?
The answer is yes!.....and no.
Some mothers can get away tear-free, but for some, the perineum has to give.
Depending on your situation and the baby’s size, four grades of perineal tears can happen.

Photo from Baby Center
When you’ve given birth through vaginal delivery, you will experience all sorts of soreness down there postpartum. Apart from vaginal soreness, you should be able to take care of your perineal lacerations.
Who’s likely to get perineal lacerations?
Tenderness
After your delivery, your body works hard to make room for the changing needs of the baby while simultaneously reverting your body back to normal. The most tender parts of your body during this time will be your belly and your breasts.
Regardless if you’re breastfeeding or not, you will experience breast engorgement since you are producing milk which will make your breasts swollen and tender.
Uterine Contractions
Along with tender breasts, your belly will also feel tender and painful with both sharp and dull sensation which often gets worse when you’re breastfeeding. This is because when you’re breastfeeding, the hormone oxytocin is released which helps contract your uterus to its normal size while keeping blood loss in check. While this sensation is extremely uncomfortable, its your body’s way of morphing into the needs of you and your baby.
Not only that, but did you know your uterus expands up to 500 times its pre-pregnancy size to nourish and make room for the baby? So yes, your body is hard at work at shrinking your uterus back to its normal size by cramping your soft muscles through each pulsating sensation.
You can ask for painkillers from your nurse or midwife if you can’t take the pain. You can also use a heating pad or ice pack depending on your situation. If it doesn’t get better, contact your doctor immediately.
Incontinence
As you know by this point, your body is just slowly adjusting back to your pre-pregnancy body. Your body has adjusted so much to nourish your little one. As the days progress and your baby descends, there’s more pressure placed on your pelvic floor muscles and bladder. When the baby comes out, these muscles have been weakened throughout the pregnancy.
Along with the hormonal changes that happen in your body’s effort to bring back your body pre-pregnancy, it can put pressure on your bladder. Without the size of the baby holding your muscles, everything might feel a little loose and might not be able to hold abrupt sensations like sneezing, laughing, or exercise.
Discharge
Vaginal Discharge
Lochia is what you call your vaginal discharge after you give birth. It’s basically what was inside your uterus. It’s normal to be red and may sometimes contain blood clots. This can last for a few weeks or a few months.
Breast Discharge
Once you’ve given birth, you’ve officially become a milk machine where the slightest cry or thought of your baby prompts you to lactate. This can continue up to 3 years after nursing.
Hemorrhoids
Apart from possible perineal lacerations, you may experience hemorrhoids.
As your baby grows during the pregnancy, the baby puts pressure on your rectal area. This makes hemorrhoids a common occurrence for moms during their pregnancy and after. Hemorrhoids can be easily relieved by home remedies but if you experience excessive bleeding, contact your healthcare provider immediately.
Constipation
Constipation after a C-section surgery is quite common. Sometimes it’s caused nerves because some people are anxious about putting force on their anus. Other times it’s the side effect of epidural or pain killers you’ve taken before.
If you’ve had an episiotomy, there is even more apprehension to pass stool after delivering a baby. If you're worried about constipation, know that you can ask for stool softeners to make passing stool easier for you and to make sure that you won’t feel any pain.
All the essentials for postpartum will most likely be provided by the hospital including a mesh underwear, pads, numbing spray, a peri bottle, and baby’s first clothes.
However, there are a few more things that might make your life easier during your delivery. You may need a few more things:
 |
|
ICEWRAPS INSTANT PERINEAL COLD PACK - 2 IN 1 ABSORBENT MAXI PAD AND INSTANT COLD PACK
|
It’s hard to predict how long labor will be so while you’re at the hospital, you might as well make yourself at home.
Though it may feel like you’re recovered within the 6 to 8 week mark, fully healing will really take time and may take 6-12 months until you’re fully okay. It’s important to baby yourself during the first week postpartum. As your mama bear instincts kick in, remember that you’re still in recovery yourself. Don’t try to do it all and honor your body’s way of healing.
Here are some things that you can and can’t do as you go through postpartum recovery.
Some symptoms to look out for include:
Mothers with a pre-existing mental health issue like depression or bipolar disorder have a higher predisposition to postpartum depression. If you wanna check if you have postpartum depression, you refer to the Edinburg postnatal depression scale to measure your symptoms. As always, reach out to your healthcare provider for help.
Your body has expanded and adjusted in order to carry your baby for months. After delivering your bundle of joy to the world, give your body the rest and time it needs in order to recuperate. Take care of yourself as you would your little one.
Support yourself through every cramp and soreness with IceWraps Instant Perineal Packs. Stock up on this postpartum essential in your hospital bag and at home.

|

|
|
ICEWRAPS INSTANT PERINEAL COLD PACK - 2 IN 1 ABSORBENT MAXI PAD AND INSTANT COLD PACK |
ICEWRAPS 4X10 REUSABLE MULTIPURPOSE HOT/COLD GEL PACK |

|

|
Comments will be approved before showing up.